Among COVID-19 exposed individuals, people in their 70s have roughly twice the mortality of those in their 60s, 10 times the mortality of those in their 50s, 40 times that of those in their 40s, 100 times that of those in their 30s, 300 times that of those in their 20s, and a mortality that is more than 3000 times higher than for children. Since COVID-19 operates in a highly age specific manner, mandated counter measures must also be age specific. If not, lives will be unnecessarily lost.
To determine effective public health counter measures against COVID-19, it is important to know the population characteristics of the epidemic [1]. It has been widely reported that mortality rates among those diagnosed and hospitalized are higher in older age groups [2, 3], but to determine public health action, it is the mortality among those exposed or infected that is of primary importance. Absolute risk estimates are uncertain at this stage of the epidemic, due to asymptomatic infected individuals [4] and limited population based testing [1], but with reasonable assumptions about exposure, it is possible to obtain rough estimates of the relative risks in different age groups, as well as upper bounds for the absolute risks.
We consider two alternative exposure scenarios at the early stages of the outbreak in Wuhan, before any social distancing was in place. In Scenario A, the likelihood of being exposed was equal in all age groups. In Scenario B, those <70 had twice the exposure compared to ages 70-79, who in turn had twice the exposure of those 80 and older. The truth probably lies somewhere in between these two scenarios.
Using Wuhan data for the relative risk of a COVID-19 diagnosis after exposure (RRC|E) and national Chinese data for the relative risk of death after a diagnosis (RRD|C) [2], the estimated relative risk of death among those exposed is RR = RRC|E x RRD|C. The Wuhan data better reflect the pre-social distancing phase of the epidemic while the Chinese mortality data increase the sample size of diagnosed individuals, generating more reliable estimates.
With age 70-79 as baseline, relative mortality risks are shown in Table 1. For COVID-19 exposed individuals, people in their 70s have roughly twice the mortality of those in their 60s, 10 times the mortality of those in their 50s, 40 times that of those in their 40s, 100 times that of those in their 30s, 300 times that of those in their 20s, and a mortality that is more than 3000 times higher than for children. Under Scenario B, with higher exposure among the young, the age differences are even larger.
In the United States, social distancing was in place early on, and since it is easier for retired people to stay home, it is likely that there was much less exposure among older people. Despite this, there is a higher proportion of diagnosed cases among the older population [5]. This means that the U.S. numbers are consistent with those from China.
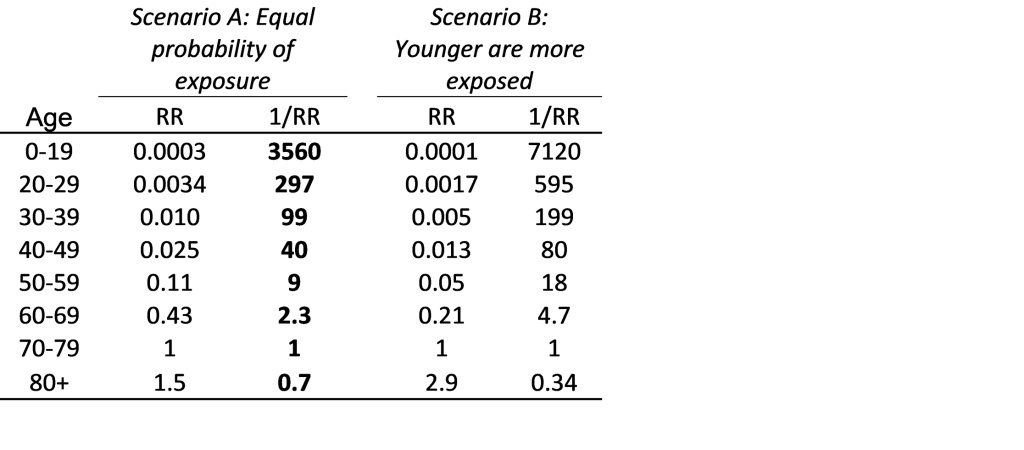
Table 1: Relative risks (RR) for COVID-19 mortality by age group. In scenario A, pre-social distancing probability of exposure is assumed to be equal across all ages. In scenario B, it is assumed to be twice as high for those <70 and half as much for those >80, compared to age 70-79.
Since 1/RR is approximately 100 for age 30-39, exposure of only 1,000 people in their 70s would lead to the same number of deaths as the exposure of 100,000 persons in their 30s. In other words, in order to avoid the same fixed number of deaths, one must prevent COVID-19 exposure to 1,000 people in their 70s, or 10,000 people in their 50s, or 40,000 in their 40s, or 100,000 in their 30s, or 300,000 in their 20s, or 3.5 million children. Preventing exposure of 3.5 million children or 100,000 people in their 30s is practically, logistically, and financially more challenging than preventing exposure of 1,000 people aged 70-79.
Government officials would be wise to take advantage of these widely different mortality rates by age in devising their COVID-19 counter measures, while still maintaining essential societal services. Whether mandated counter measures are intensified, recalibrated, or gradually relaxed sometime in the future, age specific measures should be part of the strategy. If not, there will be unnecessary mortality, burden on hospitals and economic disruption. Counter measures directed specifically at older people will not only protect them, it will also free up health care resources for those younger people that do need hospital care.
To date, most government mandated mitigation measures have either been age neutral, such as restaurant closures, or targeted at young and middle-aged people, such as school and office closures. A more appropriate age targeted approach is needed. Just as some pubs ban customers under the age of 21, government officials could set temporary upper age limits of say 50, 60, or 65 for visiting or working at restaurants, stores, offices, airports, and other public places. So, for example, while all 60-plus-year-old supermarket cashiers, gas station attendants, police officers, postal workers, garbage collectors and bus drivers should stay home, their younger colleagues should keep working, taking extra shifts as needed.
Counter measures must consider not only relative risks but also absolute risks. Among diagnosed cases age 70-79, the mortality rate in China was 1 in 25. [2] Their absolute mortality risk when simply exposed is then less than that, although we do not know how much less. Transformed to other age groups, using the data from Table 1, the absolute risk-of-death point estimates among those exposed is less than 1 in 25×3560=89,000 for children, less than 1 in 7,500 for age 20-29, less than 1 in 2,500 for age 30-39, less than 1 in 1,000 for age 40-49, less than 1 in 230 for age 50-59, less than 1 in 58 for age 60-69, less than 1 in 25 for age 70-79 and less than 1 in 17 for those in the 80+ age group. These numbers for exposed individuals are more favorable but similar to recent mortality estimates for infected individuals [3]. To put these upper bounds in context, the upper bounds for children and young adults are lower than the U.S. infant mortality rate of 1 in 170 or the annual child mortality rate of around 1 in 6,000 [6]. For the older age groups, on the other hand, the upper bounds on the mortality rates are staggeringly high.
Infectious disease outbreaks have occurred throughout history and will continue to do so, aided by urbanization and long-distance travel. COVID-19’s ability to kill and its rapid spread make it a formidable enemy that is impossible to stop until herd immunity is reached. Just as in war, we must exploit the characteristics of the enemy in order to defeat it with the minimum number of casualties. Since COVID-19 operates in a highly age specific manner, mandated counter measures must also be age specific. If not, lives will be unnecessarily lost.
Martin Kulldorff, Biostatistician, Professor of Medicine, Harvard Medical School, Boston
References
[1] M. Lipsitch, D. L. Swerdlow och L. Finelli, ”Defining the Epidemiology of Covid-19 — Studies Needed,” New England Journal of Medicine, vol. 382, pp. 1194-1196, 2020.
[2] J. T. Wu, K. Leung, M. Bushman, N. Kishore, R. Niehus, P. M. d. Salazar, B. J. Cowling, M. Lipsitch och G. M. Leung, ”Estimating clinical severity of COVID-19 from the transmission dynamics in Wuhan, China,” Nature Medicine, pp. 1-5, 2020.
[3] R. Verity, L. C. Okell, I. Dorigatti, P. Winskill, C. Whittaker, N. Imai, G. Cuomo-Dannenburg och etal, ”Estimates of the severity of coronavirus disease 2019: a model-based analysis,” The Lancet Infectious Diseases, 2020.
[4] R. Li, S. Pei, B. Chen, Y. Song, T. Zhang, W. Yang och J. Shaman, ”Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV2),” Science, nr March 16, 2020.
[5] CDC COVID-19 Response Team, ”Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-19) — United States, February 12–March 16, 2020,” Morbidity and Mortality Weekly Report, vol. 69, nr 12, pp. 343-346, 2020.
[6] S. L. Murphy, J. Xu, K. D. Kochanek och E. Arias, ”Mortality in the United States, 2017,” National Center for Health Statistics, Hyattsville, MD, USA., 2018.
Originally published on LinkedIn
Join the conversation:

Published under a Creative Commons Attribution 4.0 International License
For reprints, please set the canonical link back to the original Brownstone Institute Article and Author.









