In late 2020, the airways became saturated with triumphant reporting of Pfizer and Moderna’s “95% effective” covid-19 vaccines. Millions rolled up their sleeves with the belief that reaching herd immunity would end the pandemic.
But by June 2021, the pandemic endgame story had gone off script. Highly vaccinated countries like Israel were experiencing a new wave of covid infections, vaccination rates were starting to slow, and public scepticism was snowballing.
Authorities tried to allay fears by saying that new infections were “rare breakthroughs,” but the data became too difficult to ignore.
By early July, the Israeli Ministry of Health reported that vaccine effectiveness against infection and symptomatic disease had fallen to 64 percent. Three weeks later, revised estimates put Pfizer’s vaccine at just 39 percent effective.
Delayed disclosure
Regulatory filings date stamped from April 2021 show Pfizer had strong evidence that its vaccine’s efficacy waned – results the company did not publicly release until the end of July.
Peter Doshi, associate professor at the University of Maryland School of Pharmacy, accessed these documents from the Canadian drug regulator, Health Canada.
“It’s clear from the documents that these analyses were almost four months old by the time they became public,” said Doshi.
“It’s disappointing that neither Pfizer, nor regulators, disclosed these data until it was too obvious to ignore new outbreaks in Israel and Massachusetts, which made it clear that vaccine performance was not holding up.”
When mRNA vaccines were first authorised in 2020, FDA scientists had listed critical ‘gaps’ in the knowledge base. Two of them were effectiveness against viral transmission and duration of protection.
But on April 1, 2021, when Pfizer announced its 6-month data from its Phase III trial, there was no mention of waning immunity by Pfizer or the regulators. On the contrary, officials repeated standard talking points.
Speaking on national TV, Anthony Fauci told the American public that “when you get vaccinated, you not only protect your own health … you become a dead end to the virus.”

Then, on a door-to-door vaccination drive, Fauci told one unvaccinated resident, “on the very, very, very rare chance that you do get it even if you’re vaccinated … you don’t even feel sick, it’s like you don’t even know you got infected.”
Martin Kulldorff, biostatistician, and professor of medicine at Harvard (on leave) says he is disappointed with the lack of transparency.
“In public health, it is important to be honest with the public. Pfizer should have reported the declining vaccine efficacy in its April 1, 2021 press release, which they clearly knew about at the time,” said Kulldorff.
Pfizer gave no explanation for why it delayed the publication of its data. The FDA did not confirm when it first learned about waning efficacy and Health Canada did not respond by the deadline.
Outcome of hiding data?
In that four-month delay, approximately 90 million Americans queued to get vaccinated (see graph), unaware that data were already in hand, hinting that two doses may not be the final ask.
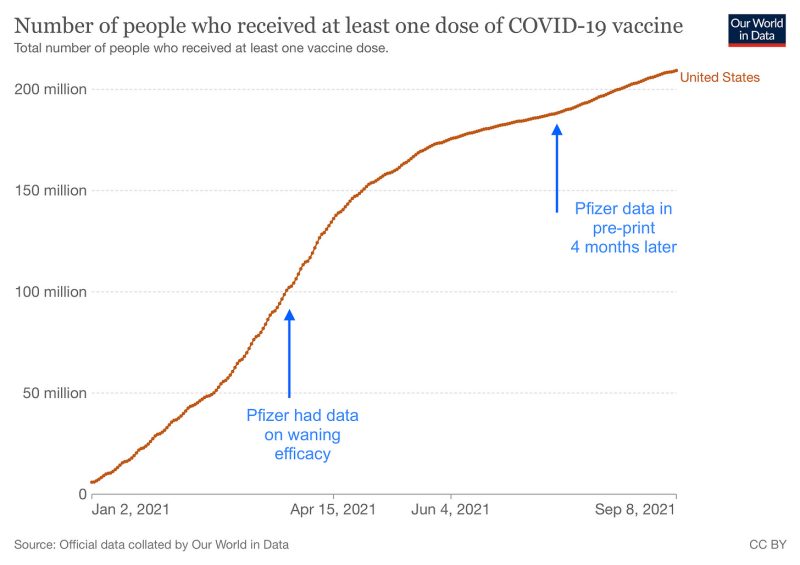
Doshi speculated that if the public was told about waning efficacy in April 2021, it may have hampered a vaccination campaign that had enormous momentum.
“Publicly disclosing that efficacy waned so soon after authorisation might have undermined the credibility of authorities, who’d been projecting great confidence about the vaccines’ ability to end the pandemic,” said Doshi.
“Also, the safety evaluation was based on a course of two doses, so publishing data that might jumpstart a conversation about people needing extra doses, could certainly have raised questions about vaccine safety,” added Doshi.
Within weeks of Pfizer publishing its data on waning efficacy, President Biden mandated all federal workers (and employees of contractors) to get vaccinated within 75 days, otherwise they’d face punishment or have their employment terminated.
Republished from the author’s Substack
Join the conversation:

Published under a Creative Commons Attribution 4.0 International License
For reprints, please set the canonical link back to the original Brownstone Institute Article and Author.









